Gynaecologic Oncology
Gynaecologic Oncology (often shortened to Gynae-Onc) is the branch of medicine dedicated to treating cancers of the female reproductive system.
Think of it as a “super-specialty.” A general gynaecologist handles routine women’s health (like periods, pregnancy, and birth). A Gynaecologic Oncologist is a surgeon who has undergone additional years of specialized training specifically to diagnose, treat, and manage cancers in these organs.
1. The "Big 5" Cancers
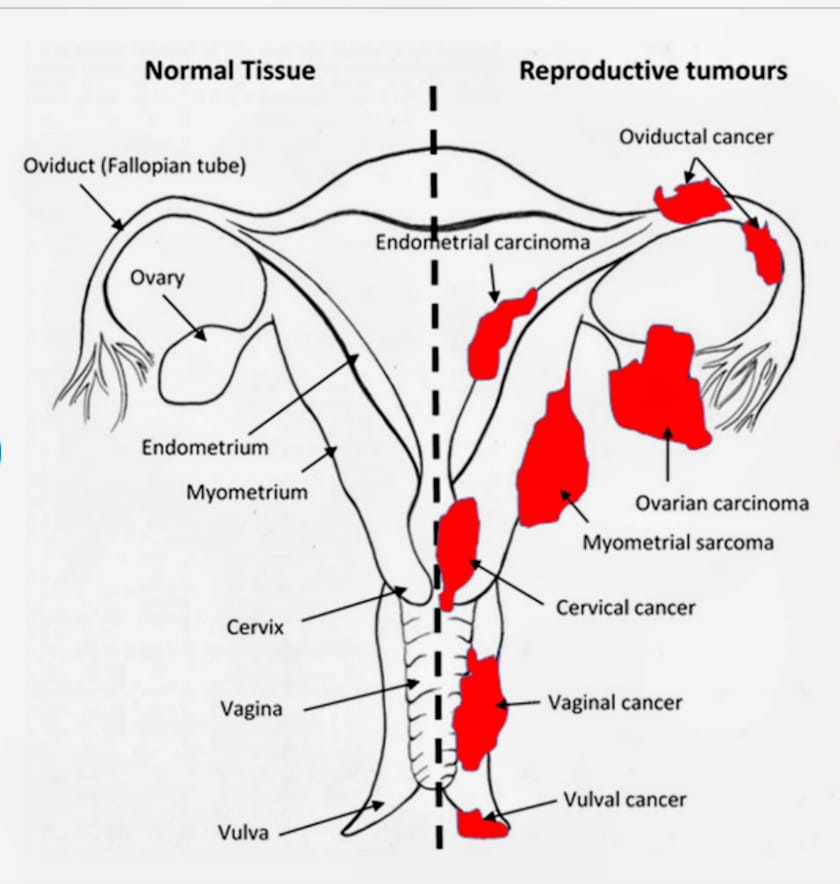
Gynaecologic oncology focuses on cancers in five specific areas of the female body:
1. Ovarian Cancer: Affects the ovaries (where eggs are produced). It can be hard to detect early because symptoms like bloating are vague.
2. Uterine (Endometrial) Cancer: Affects the lining of the womb (uterus). It is the most common type and often presents with abnormal bleeding.
3. Cervical Cancer: Affects the cervix (the neck of the womb). This is highly preventable due to vaccines (HPV) and screening (Pap smears).
4. Vaginal & Vulvar Cancers: These are much rarer and affect the external genitalia or the birth canal.
What Makes the Doctor Special?
In many other types of cancer, you might see one doctor for surgery and a different doctor for chemotherapy.
1. The Unique Role: Gynaecologic Oncologists are unique because they are trained to do both. They perform the complex surgeries required to remove tumors, and they often manage the chemotherapy or medical treatment plans as well.
2. Continuity: This means a patient often stays with the same main doctor from diagnosis through surgery and recovery.
Common Warning Signs
While symptoms vary by cancer type, there are general “red flags” that Gynaecologic Oncologists look for:
1. Abnormal Bleeding: Bleeding after menopause, bleeding between periods, or very heavy periods.
2. Pelvic Pain or Pressure: Persistent pain in the abdomen or pelvis that doesn’t go away.
3. Bloating: Feeling full quickly or persistent bloating (common in ovarian issues).
4. Changes in Bathroom Habits: Urgent need to pee or constipation without a clear cause.
How Is It Treated?
Treatment usually involves a combination of three approaches:
1. Surgery: To remove the cancer. This can range from minimally invasive “keyhole” (laparoscopic/robotic) surgery to major open surgery, depending on the stage.
2. Chemotherapy/Radiation: Using medicine or high-energy rays to kill remaining cancer cells.
3. Targeted Therapy: Newer medicines that attack specific weakness in cancer cells (e.g., genetic mutations).
Prevention is Key
A major part of this field is stopping cancer before it starts.
1. Pap Smears/HPV Testing: Screening can catch cervical changes before they turn into cancer.
2. HPV Vaccine: Protects against the virus that causes the majority of cervical, vaginal, and vulvar cancers.
3.Family History: If breast or ovarian cancer runs in the family (e.g., BRCA genes), these specialists help manage that risk.
Would you like to know more about the specific symptoms for one of these types, or how the screening process works?
