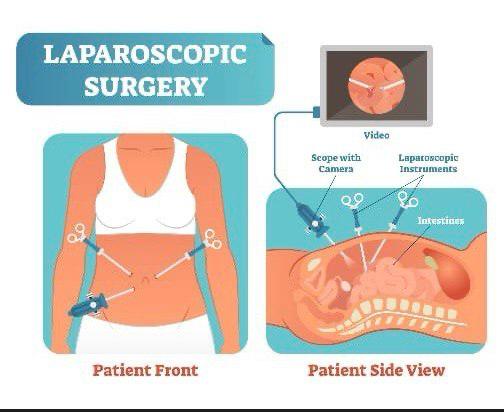
Laproscopic Surgery
Gynecological laparoscopic surgery, also known as keyhole surgery or minimally invasive surgery (MIS), is a modern surgical technique used to diagnose and treat conditions affecting a woman’s reproductive organs (uterus, ovaries, fallopian tubes, etc.).
It is considered an alternative to traditional “open” surgery, which requires a large incision.
What is Laparoscopic Gynecological Surgery?
The key features of this procedure are:
1. Minimally Invasive: The surgeon operates through one or a few very small incisions, typically 0.5 to 1.5 centimeters long, often near the belly button and lower abdomen.
2. Laparoscope: A thin, lighted tube with a camera (a laparoscope) is inserted through one of the small incisions. The camera transmits magnified images of the internal organs to a video monitor, guiding the surgeon.
3. Specialized Instruments: Very fine surgical instruments are inserted through the other small incisions to perform the procedure.
4. Insufflation: Carbon dioxide gas is often pumped into the abdomen to inflate the area, which lifts the abdominal wall away from the organs and creates a clear working space for the surgeon.
Benefits Compared to Open Surgery
Laparoscopic surgery is often preferred due to its significant advantages:
1. Smaller Incisions and Less Scarring: The small “keyholes” result in tiny, less noticeable scars.
2. Less Pain: Reduced trauma to the abdominal wall generally leads to less post-operative pain.
3. Shorter Hospital Stay: Many patients are discharged the same day or the next morning.
4. Faster Recovery: Patients can often return to daily activities and work more quickly.
5. Reduced Risk of Complications: This includes less blood loss, a lower risk of infection, and a reduced risk of forming scar tissue (adhesions).
Diagnostic Uses (Finding the Cause)
A diagnostic laparoscopy is often performed when non-invasive tests (like ultrasound or blood work) cannot confirm the cause of a patient’s symptoms.
1. Unexplained Pelvic Pain:
To visualize the organs directly and identify sources of chronic pain, such as scar tissue (adhesions) or endometriosis.
2. Investigating Infertility:
To check for blockages in the fallopian tubes, assess the extent of endometriosis, or look for other anatomical issues that could be preventing conception.
3. Evaluation of Mass/Cyst:
To examine an ovarian cyst, mass, or tumor for signs of malignancy or to guide the next steps in treatment.
4. Diagnosis of Chronic Pelvic Inflammatory Disease (PID):
To confirm the diagnosis, assess the severity, and look for associated abscesses.
Therapeutic Uses (Treatment)
| Condition Treated | Laparoscopic Procedure | Purpose |
|---|---|---|
| Uterine Fibroids | Myomectomy | To remove fibroids while preserving the uterus for future fertility. |
| Endometriosis | Excision/Ablation | To remove or destroy endometrial implants and scar tissue (adhesions). |
| Ovarian Cysts/Tumors | Ovarian Cystectomy | To remove the cyst while preserving the ovary. |
| Uterine Conditions | Hysterectomy | To remove the entire uterus (and sometimes the fallopian tubes and/or ovaries). |
| Ectopic Pregnancy | Salpingectomy / Salpingostomy | To remove a pregnancy implanted outside the uterus, usually in the fallopian tube. |
| Female Sterilization | Tubal Ligation | To block or cut the fallopian tubes to permanently prevent pregnancy. |
| Scar Tissue | Adhesiolysis | To cut and remove scar tissue (adhesions) causing pain or fertility issues. |
| Pelvic Organ Prolapse | Sacrocolpopexy / Suspension | To repair and suspend prolapse. |
